Hormone Therapy for Cancer is a powerful treatment that slows or stops hormone-sensitive tumors. If you face a recent diagnosis, understanding your options is vital for recovery.
This guide explores how these targeted treatments work, detailing the various types, proven benefits, and potential side effects. We provide actionable advice, expert insights, and a comprehensive FAQ section to help you confidently navigate your treatment journey and improve your overall well-being.
Understanding Hormone Therapy for Cancer
Hormone Therapy for Cancer, often referred to as endocrine therapy, is a targeted medical approach used primarily for cancers that rely on natural hormones to grow and spread. These include specific subtypes of breast cancer and prostate cancer. By interfering with hormone production or blocking hormone receptors on cancer cells, this treatment effectively starves the tumor of the fuel it needs to multiply.
How the Treatment Works
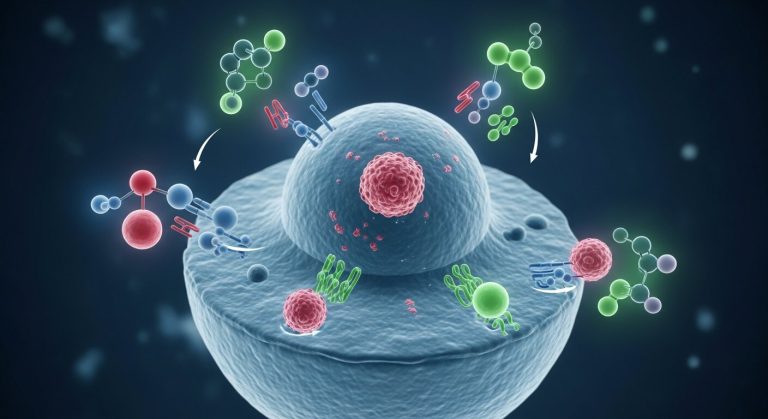
Certain cancer cells contain specific receptors that bind to hormones like estrogen, progesterone, or testosterone. When these hormones attach to the receptors, they send signals that tell the cancer cells to grow and divide. Hormone Therapy for Cancer works in two primary ways:
- Blocking Receptors: Some medications attach themselves to the hormone receptors on the cancer cells, creating a physical barrier that prevents natural hormones from binding.
- Lowering Hormone Production: Other therapies stop the body from producing specific hormones altogether, usually by targeting the ovaries or testicles, or by inhibiting the enzymes in fat tissue that produce hormones after menopause.
Who is a Candidate?
Not all cancers respond to hormone manipulation. Your medical team will perform a biopsy to test your tumor for hormone receptors. If your breast cancer tests positive for estrogen receptors (ER-positive) or progesterone receptors (PR-positive), or if you are diagnosed with prostate cancer (which relies on testosterone), you are likely a candidate for Hormone Therapy for Cancer. Tumors that lack these receptors will not benefit from this specific approach and require different targeted therapies or chemotherapy.
a candidate for Hormone Therapy for Cancer. Tumors that lack these receptors will not benefit from this specific approach and require different targeted therapies or chemotherapy.
Types of Hormone Therapy for Cancer
The specific type of Hormone Therapy for Cancer prescribed to you depends on your cancer type, stage, biological sex, and menopausal status.
Medications That Block Hormones
These drugs circulate through your bloodstream and bind to hormone receptors on cancer cells. For breast cancer, the most common category is Selective Estrogen Receptor Modulators (SERMs). Tamoxifen is a widely used SERM that blocks estrogen from attaching to breast cancer cells while acting like estrogen in other tissues, such as bones. Selective Estrogen Receptor Degraders (SERDs), like Fulvestrant, go a step further by not only blocking the receptor but also causing it to break down entirely. For prostate cancer, anti-androgens (like Bicalutamide or Enzalutamide) bind to testosterone receptors to prevent tumor growth.
Aromatase Inhibitors (AIs)
Aromatase inhibitors are specifically used for postmenopausal women with breast cancer. After menopause, the ovaries stop producing estrogen, but the body continues to make small amounts in fat tissue and muscle using an enzyme called aromatase. AIs, such as Letrozole, Anastrozole, and Exemestane, block this enzyme, drastically lowering the total amount of estrogen in the body. Because they do not block ovarian estrogen, they are generally ineffective for premenopausal women unless combined with ovarian suppression.
Organ Suppression and Surgery
For some patients, stopping the main source of hormone production is the most effective Hormone Therapy for Cancer.
- For Women: Ovarian suppression can be achieved surgically by removing the ovaries (oophorectomy) or medically using Luteinizing Hormone-Releasing Hormone (LHRH) agonists like Goserelin. This puts premenopausal women into temporary or permanent menopause.
- For Men: Testicular suppression reduces testosterone levels. This is done through surgical removal of the testicles (orchiectomy) or via medications that stop the brain from signaling the testicles to produce testosterone.
Comparison Table: Common Hormone Therapies
|
Therapy Type |
Target Audience |
Primary Function |
Common Drug Names |
|---|---|---|---|
|
SERMs |
Pre & Postmenopausal Women |
Blocks estrogen receptors on cancer cells |
Tamoxifen |
|
Aromatase Inhibitors |
Postmenopausal Women |
Stops estrogen production in fat tissue |
Letrozole, Anastrozole |
|
LHRH Agonists |
Premenopausal Women & Men |
Suppresses ovarian/testicular hormone production |
Goserelin, Leuprolide |
|
Anti-Androgens |
Men with Prostate Cancer |
Blocks testosterone receptors on cancer cells |
Bicalutamide, Enzalutamide |
The Benefits of Hormone Therapy for Cancer

Opting for Hormone Therapy for Cancer provides significant systemic benefits, especially for early-stage and locally advanced hormone-receptor-positive cancers.
Preventing Cancer Recurrence
One of the most profound benefits of this therapy is its ability to keep cancer from coming back. Taking hormone blocking medications for a prescribed period—typically 5 to 10 years after primary treatments like surgery or radiation—reduces the risk of recurrence by almost half. This long-term protective effect makes it a cornerstone of comprehensive cancer care.
Improved Long-Term Survival Rates
By consistently starving any remaining microscopic cancer cells of the hormones they need to survive, Hormone Therapy for Cancer significantly improves long-term overall survival rates. It is highly effective at preventing the spread of cancer to other organs (metastasis).
A Non-Cytotoxic Approach
Unlike traditional chemotherapy, which attacks all rapidly dividing cells in the body (leading to hair loss, severe nausea, and a weakened immune system), hormone treatments are targeted. They specifically affect hormone-sensitive tissues, meaning they are non-cytotoxic. This allows many patients to maintain a better quality of life and continue their daily routines while undergoing treatment.
Potential Side Effects of Hormone Therapy for Cancer
While generally better tolerated than chemotherapy, Hormone Therapy for Cancer disrupts the body’s natural endocrine balance, leading to noticeable side effects. Recognizing and managing these symptoms is crucial for maintaining your quality of life.
Common Side Effects in Women
Because these therapies induce or mimic menopause, women often experience:
- Hot flashes and night sweats: Sudden, intense feelings of heat.
- Bone density loss: Aromatase inhibitors, in particular, can lead to osteoporosis or osteopenia, increasing the risk of fractures.
- Joint and muscle pain: Stiffness and aching, particularly in the mornings.
- Vaginal dryness and sexual dysfunction: Decreased libido and discomfort during intimacy.
- Mood swings and fatigue: Hormonal shifts can cause irritability, depression, and persistent tiredness.
Common Side Effects in Men
Men receiving androgen deprivation therapy for prostate cancer may experience:
- Hot flashes: Similar to those experienced by women.
- Loss of libido and erectile dysfunction: A direct result of lowered testosterone.
- Fatigue and loss of muscle mass: Reduced energy levels and physical strength.
- Breast tenderness and enlargement: A condition known as gynecomastia.
- Metabolic changes: Increased risk of weight gain, diabetes, and cardiovascular issues.
Rare but Serious Risks
Certain medications carry rare but serious risks. For instance, Tamoxifen can slightly increase the risk of blood clots, stroke, and endometrial cancer in postmenopausal women. Your healthcare provider will continuously monitor you to mitigate these risks. Check authoritative resources like the American Cancer Society for detailed drug-specific profiles.
Your Treatment Guide: Navigating the Journey

Starting a multi-year treatment plan can feel overwhelming. A structured approach helps you manage the physical and emotional demands of Hormone Therapy for Cancer.
Preparing for Treatment
Before starting, have a comprehensive discussion with your oncologist. Ask about the specific medication, the optimal duration of therapy, and what side effects to anticipate. Consider getting a baseline bone density scan (DEXA scan) and a thorough cardiovascular check-up. Establish a strong support system, whether through local community groups, counseling, or online patient networks.
Managing Side Effects Proactively
You do not have to suffer in silence. If side effects are severely impacting your life, tell your medical team immediately. They can often prescribe secondary medications to manage hot flashes or joint pain, or they might suggest switching you to a different hormone therapy drug within the same class.
Adopt a healthy lifestyle to combat fatigue and bone loss. Incorporate weight-bearing exercises to strengthen your bones, and eat a balanced diet rich in calcium and vitamin D. For men facing muscle loss, resistance training is highly recommended to maintain physical function and metabolic health.
Expert Insights and Common Mistakes to Avoid
Success with Hormone Therapy for Cancer relies heavily on consistency and communication.
Pro Tips for Patients
- Track Your Symptoms: Keep a daily journal of your side effects. Note what triggers hot flashes or when joint pain is most severe. This data is invaluable for your doctor.
- Stay Hydrated and Active: Regular physical activity is one of the most effective ways to combat cancer-related fatigue and joint stiffness.
- Explore Integrative Therapies: Many patients find relief from hot flashes and anxiety through acupuncture, yoga, and meditation.
Common Mistakes to Avoid
- Stopping Medication Abruptly: The most dangerous mistake is quitting your medication without telling your doctor. If side effects are unbearable, communicate this. There are almost always alternative options or dose adjustments available.
- Ignoring Mental Health: The emotional toll of hormonal changes is real. Do not dismiss feelings of depression or anxiety; seek support from a licensed therapist.
- Skipping Follow-up Appointments: Regular blood tests, bone scans, and check-ups are mandatory to ensure the drug is working and to monitor for silent side effects like bone thinning.
Navigating Hormone Therapy for Cancer requires patience, deep knowledge, and open communication with your dedicated medical team. By thoroughly understanding the treatment types, benefits, and potential side effects, you can actively manage your health journey. Contact your trusted oncologist today to create a personalized care plan that maximizes your recovery.
Frequently Asked Questions
1. How long do I need to take Hormone Therapy for Cancer?
Most treatment plans require patients to take hormone therapy daily for 5 to 10 years. The exact duration depends on the specific characteristics of your tumor, the stage of your cancer, and how well you tolerate the medication. Your oncologist will assess your risk of recurrence to recommend the best timeline for you.
2. Can Hormone Therapy for Cancer cure my disease?
While it is not generally considered a standalone “cure,” it is a highly effective treatment that significantly reduces the risk of cancer returning or spreading. When combined with surgery and radiation, it drastically improves long-term survival and leads to a functional cure for many patients.
3. Will I lose my hair on hormone therapy?
Unlike traditional chemotherapy, hormone therapy does not cause total hair loss. However, some patients may experience mild hair thinning over time due to the reduction of estrogen or testosterone in the body.
4. Can I switch medications if the side effects are too severe?
Yes. If you are experiencing unbearable side effects like severe joint pain or extreme hot flashes, speak to your doctor immediately. They can often switch you to a different aromatase inhibitor or alternative hormone-blocking medication that your body might tolerate better.
5. How does hormone therapy affect bone density?
Medications that reduce overall estrogen levels, such as aromatase inhibitors and ovarian suppression drugs, can accelerate bone thinning, leading to osteopenia or osteoporosis. Your doctor will likely recommend calcium, vitamin D supplements, weight-bearing exercises, and regular bone density scans.
6. Is Hormone Therapy for Cancer the same as Hormone Replacement Therapy (HRT)?
No, they are the exact opposite. Hormone Replacement Therapy (HRT) adds hormones to the body to relieve menopause symptoms. Hormone Therapy for Cancer blocks or removes hormones from the body to stop hormone-sensitive tumors from growing.
7. Can I still get pregnant after hormone therapy?
Hormone therapy often pauses or ends a woman’s reproductive capabilities depending on age and treatment type. Because these drugs can cause severe birth defects, you should not get pregnant while taking them. If you wish to have children, discuss fertility preservation with your doctor before starting treatment.
8. Do men experience hot flashes on hormone therapy?
Yes. Men receiving androgen deprivation therapy for prostate cancer frequently experience hot flashes similar to those women experience during menopause. This occurs due to the sudden and drastic drop in testosterone levels.
9. Can I take herbal supplements to manage my side effects?
You must consult your oncologist before taking any herbal supplements or vitamins. Certain natural remedies, like black cohosh or soy-based supplements, contain phytoestrogens that can interfere with your cancer treatment and reduce its effectiveness.
10. What happens if I miss a dose of my hormone therapy pill?
If you miss a single dose, take it as soon as you remember, unless it is almost time for your next scheduled pill. Never double up to make up for a missed dose. Consistency is vital for keeping hormone levels suppressed, so setting a daily alarm is highly recommended.