Introduction
Facing a cancer diagnosis can generate significant stress for patients and families alike. In today’s digital landscape, many individuals are searching beyond standard protocols to identify methods that support both healing and quality of life. Integrative cancer treatment offers a comprehensive framework that marries evidence-informed conventional therapies—such as surgery, chemotherapy, and radiation—with holistic approaches that address mind, body, and spirit. This year (2026), healthcare practitioners increasingly recognize the importance of patient-centered care, encouraging collaboration among oncologists, nutritionists, therapists, and alternative medicine experts to devise truly personalized regimens.
By embracing integrative cancer treatment, patients can actively participate in their care, exploring therapies that reduce side effects, strengthen immune defenses, and foster mental resilience. Research institutions like the National Cancer Institute and the Centers for Disease Control and Prevention provide valuable insights into modalities that complement mainstream oncology. Throughout this article, we will examine key principles, illustrate conventional and supportive techniques, guide you in plan development, and review emerging evidence to help you navigate today’s integrative landscape.
What Is Integrative Cancer Treatment?
At its core, integrative cancer treatment unites scientifically validated medical interventions with complementary and alternative medicine (CAM) practices. Unlike standalone alternative therapies, which may replace standard care, integrative approaches augment conventional strategies to support overall well-being. In today’s health environment, patients seek more than tumor control; they desire holistic solutions that address fatigue, pain, and emotional distress.
Key principles of this model include patient-centered customization, evidence-informed decision making, collaborative multidisciplinary teams, and rigorous safety monitoring. Under this framework, each individual receives a tailored combination of treatments based on their diagnosis, treatment history, lifestyle, and personal goals. Certified integrative practitioners work alongside oncologists to ensure that herbal supplements, mind-body exercises, and nutritional adjustments interact safely with chemotherapy or radiation protocols.
Currently, studies published by leading research universities validate the impact of integrative interventions. For instance, yoga and tai chi have demonstrated reductions in anxiety and improvements in mobility among survivors, while targeted nutrition plans help mitigate treatment-related weight loss. As the scientific community continues to explore the interplay between genetics, microbiome composition, and CAM practices, integrative cancer treatment remains at the forefront of personalized medicine in today’s clinical settings.
The Role of Conventional Therapies
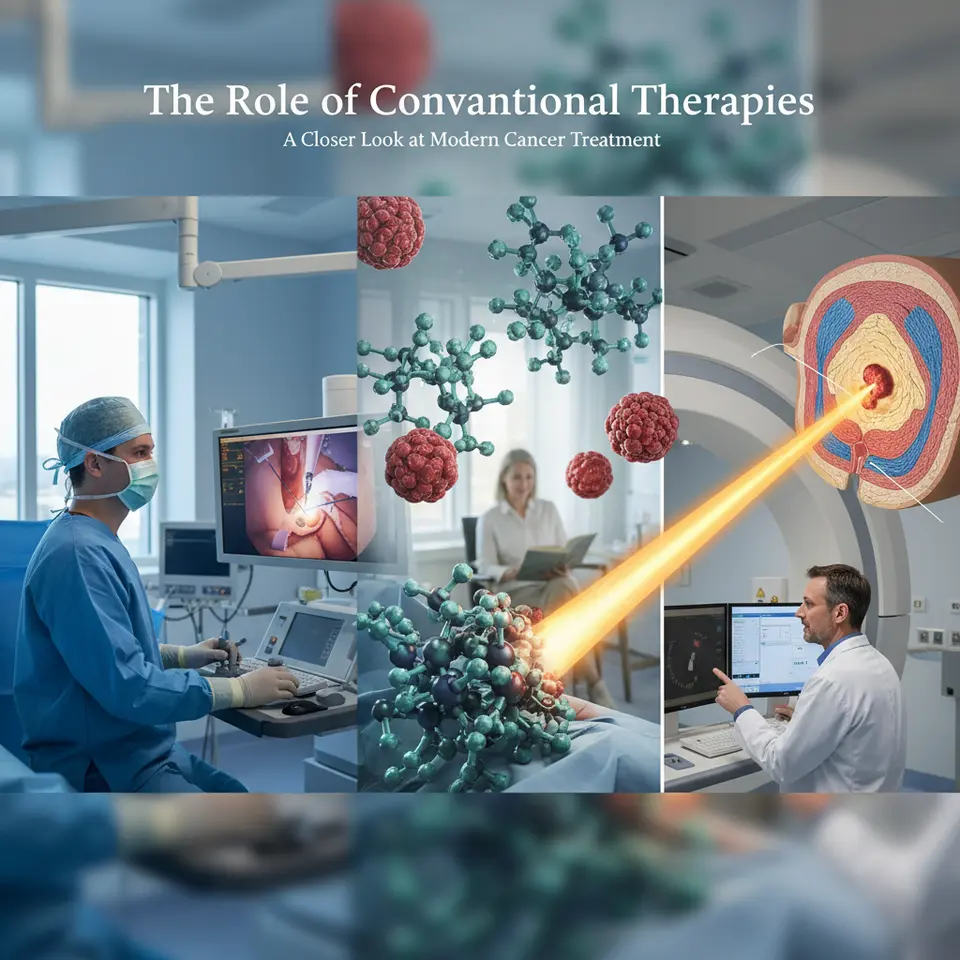
Conventional oncology treatments maintain their status as the foundation of cancer care. Integrative cancer treatment seeks to preserve the efficacy of these time-tested modalities while reducing adverse effects that can compromise patient comfort and adherence.
Surgical techniques have evolved to become less invasive, with laparoscopic and robotic-assisted procedures minimizing blood loss and speeding up recovery. These precision methods allow surgeons to excise tumors effectively while preserving as much healthy tissue as possible. Meanwhile, chemotherapy regimens have been refined to target rapidly dividing cells with greater specificity, although side effects—such as nausea, hair loss, and neuropathy—often require supportive measures to maintain patient quality of life.
Radiation therapy benefits from cutting-edge technologies like intensity-modulated radiation therapy (IMRT) and proton beam therapy. These approaches concentrate high-energy beams on cancerous tissues, limiting exposure to adjacent healthy structures. Nonetheless, fatigue and skin irritation can occur, prompting the need for integrative strategies such as acupuncture or topical herbal applications under professional guidance.
Emerging treatments—including targeted molecular therapies and immunotherapy—offer new avenues for attacking cancer at the cellular level. By identifying specific genetic mutations or harnessing the body’s immune system, these interventions may produce fewer systemic side effects compared to traditional chemotherapy. In the context of integrative cancer treatment, supportive care plans address unique toxicities associated with these novel drugs, ensuring comprehensive symptom management.
Holistic Supportive Strategies

Complementing standard treatments with holistic modalities is a defining aspect of integrative cancer treatment. These strategies focus on enhancing physical strength, mental resilience, and emotional balance to support patients throughout their journey.
Nutrition forms a critical component. Dietitians recommend nutrient-dense, anti-inflammatory foods such as leafy greens, berries, nuts, and fatty fish rich in omega-3 fatty acids. Adequate protein intake—derived from lean meats, legumes, or plant-based alternatives—supports tissue repair and immune function. Supplements like vitamin D or probiotics may benefit certain individuals, but all additions should be reviewed by the oncology team to prevent interaction risks with chemotherapy or radiation.
Mind-body interventions offer powerful tools to reduce stress and improve well-being. Practices like mindfulness meditation, guided imagery, and breathwork help lower cortisol levels and enhance emotional regulation. Physical disciplines such as yoga and tai chi promote flexibility, reduce muscle tension, and alleviate anxiety. Hypnotherapy, delivered by credentialled professionals, can address pain management and nausea control during treatment cycles.
Manual and physical therapies further support recovery. Acupuncture has been shown to decrease chemotherapy-induced nausea and peripheral neuropathy, while targeted massage can reduce lymphedema in breast cancer survivors. Personalized exercise programs—coordinated by physiotherapists—focus on strength, endurance, and balance, mitigating declines in muscle mass and cardiovascular fitness often seen during aggressive treatment phases.
Designing a Personalized Integrative Plan
Developing an individualized integrative cancer treatment plan requires a structured, collaborative process among patients and healthcare providers. Clear communication is essential to align expectations, monitor progress, and adjust interventions as needed.
The first step is a thorough assessment: medical history, current treatment protocols, lab results, and patient preferences are all documented. This comprehensive review helps identify potential areas where integrative strategies can add value without compromising safety. Next, a risk–benefit analysis evaluates the strength of scientific evidence for each complementary modality, weighing potential gains against possible interactions with standard therapies.
Multidisciplinary case conferences often involve oncologists, integrative medicine specialists, dietitians, physical therapists, and mental health professionals. Together, the team crafts a cohesive plan that may include dietary modifications, stress-reduction exercises, specific supplement regimens, and specialized therapies such as acupuncture or massage. Regular check-ins—via in-person visits or telehealth—allow for ongoing symptom tracking and lab monitoring to ensure the regimen remains both effective and safe.
As patients progress, treatment plans are modified according to response and tolerance. For example, if a patient experiences increased fatigue, the team might shift the exercise program to include low-impact activities like aquatic therapy. If digestive side effects arise, dietary components are adjusted to improve gut health. This iterative approach ensures that integrative cancer treatment remains responsive to individual needs in today’s fast-changing healthcare environment.
Evidence, Challenges, and Future Outlook
Substantial research underscores the benefits of integrative cancer treatment, yet several challenges persist. Clinical trials published in peer-reviewed journals demonstrate that mindfulness-based stress reduction improves mood and quality of life for breast cancer survivors. Similarly, studies from institutions like the National Center for Complementary and Integrative Health highlight the value of acupuncture in managing pain and nausea.
Despite these positive findings, standardizing complementary protocols remains complex. Practitioner credentialing varies across regions, and insurance coverage for CAM services is often limited. Patients must remain vigilant against unverified “miracle cures” marketed without robust evidence. Healthcare providers play a crucial role in guiding patients toward safe, evidence-based options.
Looking ahead, research in genomics, proteomics, and microbiome analysis promises to refine personalized integrative cancer treatment further. Artificial intelligence tools are being developed to predict which supportive strategies will yield the greatest benefit for individual patients. In this year (2026), collaborative efforts among academic centers, government agencies, and industry partners continue to expand our understanding of how best to integrate holistic therapies within modern oncology.
As the field evolves, maintaining open dialogue and shared decision making between patients and providers will be key. By blending proven medical interventions with complementary modalities grounded in scientific research, integrative cancer treatment stands poised to enhance both survival and life quality for those facing cancer today.
FAQ
What is the difference between integrative and alternative cancer treatments?
Integrative cancer treatment combines standard medical therapies (like surgery, chemotherapy, and radiation) with complementary approaches (such as nutrition, mind-body exercises, and acupuncture) under the guidance of oncology teams. Alternative treatments replace conventional care and often lack rigorous scientific validation.
Are complementary therapies safe alongside chemotherapy or radiation?
Many complementary practices are safe and can reduce side effects, but it’s essential to review all supplements and modalities with your oncology team. This ensures there are no interactions with your primary treatment protocols.
How do I find qualified integrative medicine practitioners?
Look for practitioners certified by recognized bodies such as the Academy of Integrative Health & Medicine or those affiliated with major cancer centers’ integrative oncology programs. Verify credentials, experience treating oncology patients, and recommendations from your healthcare providers.
Does insurance cover integrative or CAM services for cancer care?
Coverage for complementary and integrative therapies varies widely by insurer and region. Some plans may reimburse acupuncture or nutritional counseling, while others may not. Always check with your insurance provider and explore hospital-based programs that might offer sliding-scale fees.
Conclusion
In today’s healthcare setting, integrative cancer treatment represents a transformative model that prioritizes patient-centered care, safety, and evidence-based practices. By combining conventional therapies with carefully selected supportive strategies—ranging from nutritional adjustments and mind-body techniques to physical therapies—individuals can better manage side effects, strengthen resilience, and improve overall well-being. As research advances and collaborative care frameworks mature, patients have more tools than ever to tailor their treatment journey. Always consult your oncology team when considering new integrative modalities to ensure a coordinated, effective plan that aligns with your unique needs. Embracing this comprehensive approach can empower patients to take an active role in their healing process and optimize outcomes in 2026.


